Chronic care management (CCM) is a critical component of primary care that contributes to better outcomes and higher satisfaction for patients.
CHRONIC CARE MANAGEMENT (CCM):
Medicare initially provided payment for CPT code 99490 beginning January 1, 2015 to separately identify and value clinical staff time and other resources used in providing CCM.
CMS adopted 3 additional billing codes (G0506, CPT 99487, CPT 99489)
The Centers for Medicare & Medicaid Services (CMS) recognizes CCM takes time and effort.
ELIGIBLE BENEFICIARIES:
Patient have two or more chronic conditions expected to last at least 12 months or until death, that place them at significant risk of death, acute exacerbation, or functional decline .
PATIENT CONSENT:
A practitioner must obtain patient consent before furnishing or billing CCM. Consent may be verbal or written but must be documented in the medical record, and includes informing them about:
The availability of CCM services and applicable cost-sharing
Only one practitioner may be paid for CCM services for a given calendar month. This practitioner must only report either complex or non-complex CCM for a given patient for the month (not both)
The right to stop CCM services at any time (effective at the end of the calendar month)
ELIGIBLE REPORTING PRACTITIONERS:
- Physicians
- Physician Assistants,
- Clinical Nurse Specialists,
- Nurse Practitioners,
- Certified Nurse Midwives
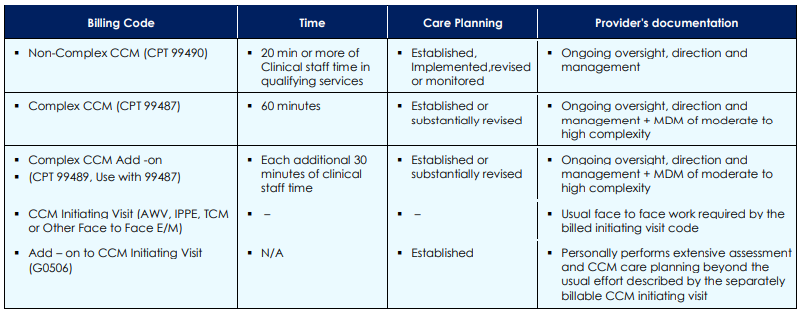
CPT CODES AND PAYMENT FOR CCM:
- CPT G0506 (Add -on code to CCM initiating visit ($ 64 )
- CPT 99490 Non complex CCM($ 43)
- CPT 99487 (Complex CCM 60 mins ($ 94)
- CPT +99489 (Complex CCM ) additional 30 mins ($ 47)
PATIENTS BENEFIT FROM CCM:
- Spend more time focusing on health and help work towards your health and Quality of life goals
- Don’t always have to come into the office to get help; you can also make a call.
- Patients will receive a comprehensive care plan.
CCM SUPPORTS OUR PRACTICE:
- Improve care coordination.
- Improve patient satisfaction and compliance, and decrease hospitalization and emergency department visits.
- Increased payment to practice for the coordinated CCM services we provide outside of face to face visits





